Sandra Beldine Otieno, MSc
September 2, 2024
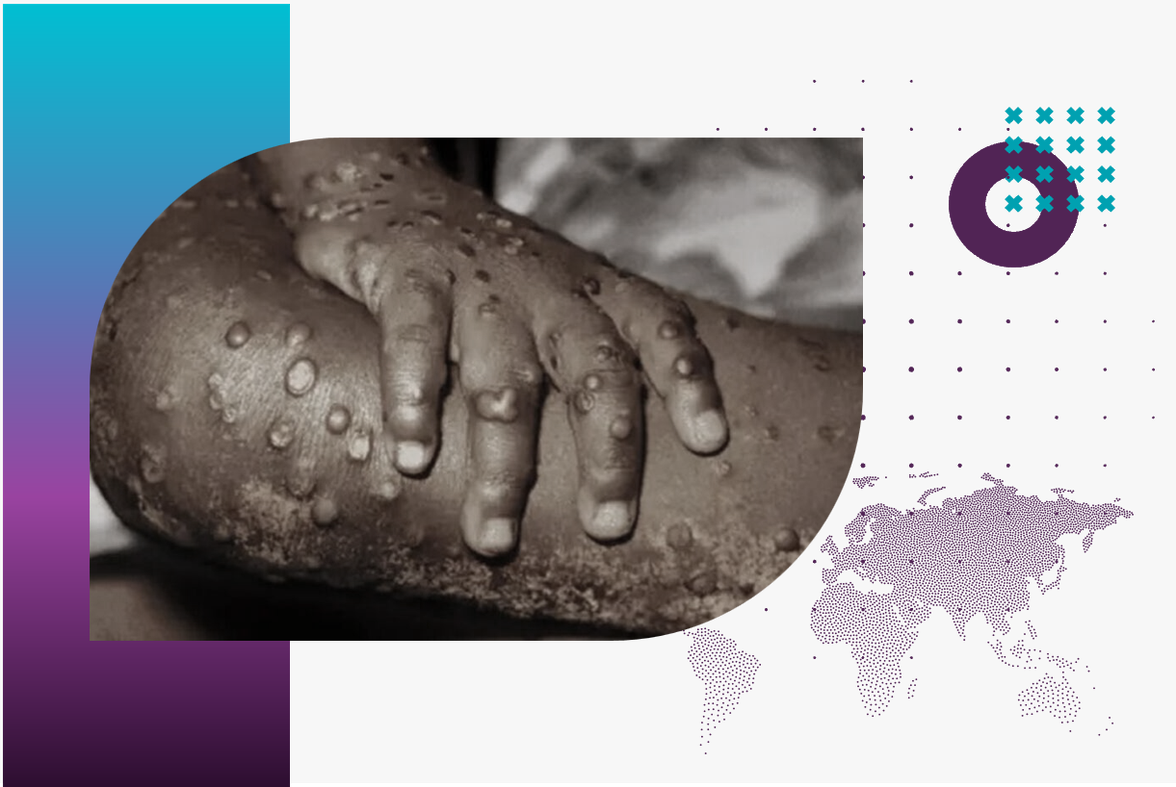
Mpox, formerly known as monkeypox, has re-emerged as a significant public health threat in Africa, exposing deep-rooted inequities in global health systems. The virus, which has been present on the continent for decades, has seen a sharp resurgence in 2024, with over 14,000 cases and nearly 500 deaths reported so far. This new wave, driven by the more virulent Clade 1b variant, has hit countries like the Democratic Republic of the Congo (DRC), Uganda, Nigeria, and Kenya particularly hard. As the outbreak unfolds, it raises urgent questions about vaccine access, public health preparedness, and the global community's response to health crises in Africa.
The 2024 mpox outbreak has been marked by a significant increase in cases and deaths, particularly in Central and East Africa. The DRC remains the epicenter, with over 10,000 cases reported and hundreds of deaths, primarily among children and vulnerable populations living in crowded conditions. Uganda, Nigeria, and Kenya have also reported a surge in cases, with community transmission spreading rapidly. The World Health Organization (WHO) has declared the outbreak a "public health emergency of international concern," prompting a global response to contain the virus's spread. Despite these efforts, the outbreak has exposed significant challenges in vaccine distribution, public awareness, and healthcare infrastructure across the continent.
One of the most pressing issues in the current outbreak is the stark inequity in vaccine access and distribution. Although several mpox vaccines have been developed and are available in Europe and the United States, African countries have faced significant delays in accessing these lifesaving tools. The WHO and global health agencies have been slow to authorize vaccine donations and emergency use licenses, citing regulatory and safety concerns. Meanwhile, the virus has continued to spread, particularly in regions with limited healthcare infrastructure and high levels of displacement due to conflict. Recent pledges of 215,000 vaccine doses from the European Union, France, Germany, and the United States are a step in the right direction but far from sufficient. Experts estimate that at least 10 million doses are needed to effectively control the outbreak, particularly given the two-dose regimen required for full immunity.
The resurgence of mpox has placed immense strain on already fragile health systems in Africa. In the DRC, ongoing conflicts have compounded the challenges of disease management, with many health facilities overwhelmed by the influx of patients. In Uganda and Nigeria, where public health infrastructure is relatively stronger, the outbreak has still highlighted significant gaps in disease surveillance and response capacity. Many rural and underserved areas lack basic medical supplies, trained staff, and diagnostic tools, making it difficult to contain the virus and prevent further spread. Misinformation and stigma surrounding the disease have also hindered public health efforts, as communities struggle to understand and trust government and international health advisories.
The mpox outbreak in Africa is not just a regional health crisis; it has significant implications for global health security and equity. The outbreak has exposed the vulnerabilities of health systems in low- and middle-income countries and underscored the need for a more coordinated and equitable global response to emerging infectious diseases. Beyond the immediate public health impact, the outbreak has exacerbated economic and social inequalities, particularly in already marginalized communities. Moving forward, it is critical for the international community to invest in strengthening health systems, improving vaccine access, and ensuring that all countries are better prepared to respond to future health emergencies.
The current mpox outbreak in Africa serves as a stark reminder of the persistent inequities in global health and the need for sustained international cooperation. While efforts to control the virus are underway, much more needs to be done to address the root causes of this and future outbreaks. By prioritizing equitable access to vaccines, investing in robust healthcare infrastructure, and fostering global solidarity, the world can better prepare for and prevent the next pandemic. Africa's experience with mpox is a powerful call to action for a more inclusive and effective global health response.
Share on socials using this caption: 🌍 Africa is battling a surge in mpox cases, revealing deep global health inequities. We need urgent action on vaccine access and stronger healthcare systems! 💉🩺 #HealthEquity #MpoxOutbreak #GlobalHealthCrisis
3847 views
Financial pressure in Ghana is shaping emotional wellbeing differently across income and age groups
The Hidden Cost of “Managing”: Egypt’s Middle Class is Trading Health for Financial Survival
Namibia's Health Landscape: From Varied Health Perceptions to Dominant Concerns